In a discussion with some colleagues recently about the future of O&P, the topics of AI, CAD/CAM, scanning, and 3D printing were mentioned as areas the profession would adopt and embrace.
Those were exactly Keith’s impressions coming out of the first O&P-specific 3D printing course he attended over 15 years ago. So why are we not further along in adopting these trends than we were then? During the conversation we explored how the barriers to adoption have decreased, allowing these trends the potential for growth in the next ten years. We also discussed whether the newest technology is so advantageous that it tips the scale for some, most, or all practitioners to pursue it.
Scanning a Model
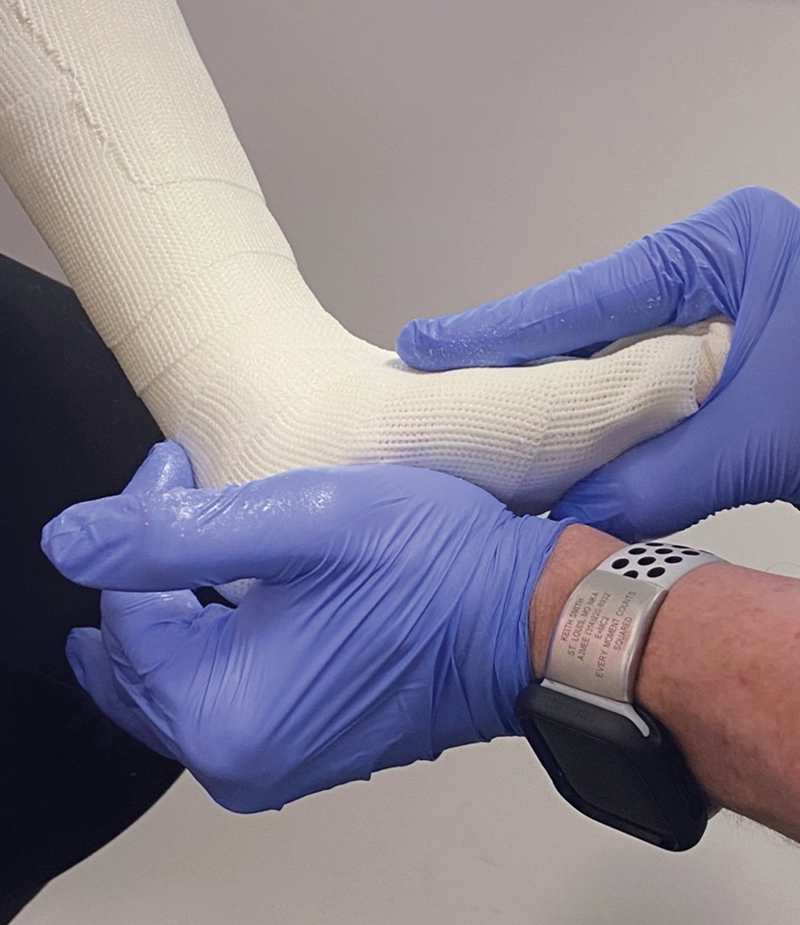
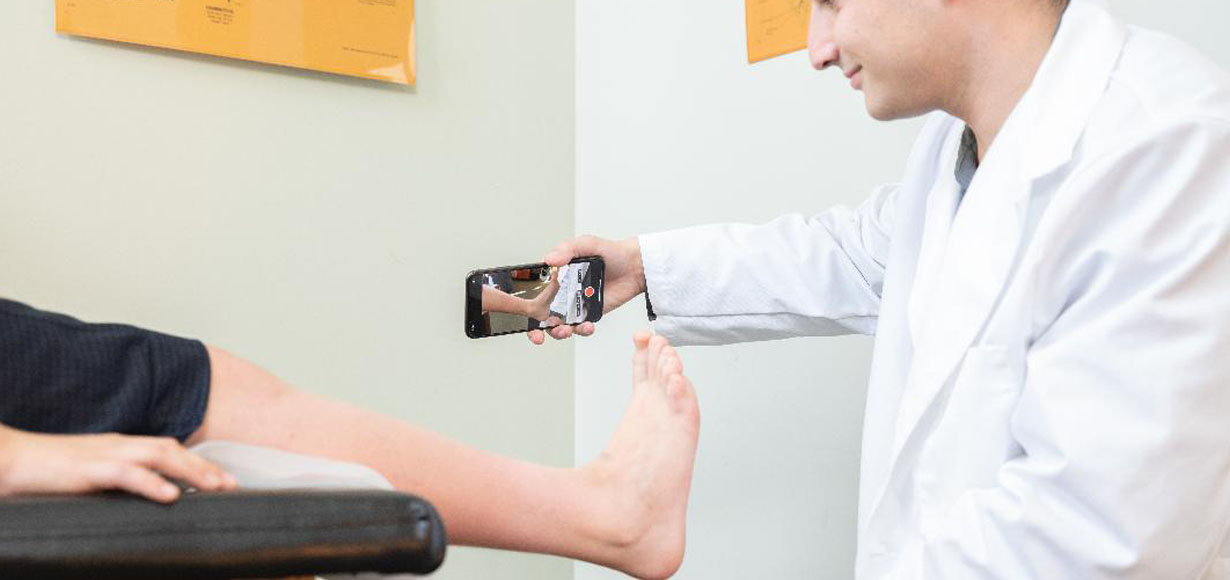
When we consider obtaining a scan, the first question to answer is at what point in the process should it be done? The earliest possible stage would be an uncorrected or mostly corrected limb without the practitioner’s hands involved. This saves time and may be the least messy for the patient, but it also may prevent the clinician from capturing the corrections that the patient can achieve. For example, a patient with cerebral palsy often needs the clinician to correct the foot and ankle complex to prevent pronation in the diplegic patient or supination in the hemiplegic patient (Figures 1 and 2). A patient with scoliosis is another good example, where it is advantageous to have the expertise to put the curve pushes into a cast mold with the use of a Risser table versus scanning an uncorrected body. If a practitioner is already taking measurements of a patient and then adding pads for the forces, then a scan may produce a better outcome than achieved by measurements alone. Keith addressed this issue in an article about a TLSO created with CAD/CAM technology at Atlantic Rim Brace Manufacturing that allowed for the traditional symmetrical TLSOs to be made asymmetrical using both scans and measurements—the earliest introduction of this approach.1
When considering uncorrected scanning versus scanning a corrected cast, the decision comes down to the patient’s presentation and the clinician’s skill and mindset. Some patient presentations may allow a scan with the desired correction, such as a patient with foot drop and very minimal transverse and coronal deviations or a foot orthotic who can hold the foot in a corrected position (Figure 3). Scanning that patient directly may be the best choice as scanning eases the work of obtaining a mold and does not sacrifice function or position. Modifications can be done digitally, which minimizes the need for guesswork. In taking a scan of an uncorrected limb and digitally adding corrections, the scan may be an easier option than casting, but we need to ask if we are still getting the function we want out of our design.
Skills Matter
In this regard, the skill level of the clinician matters. Jeff Erenstone, CPO, says, “If you’re an experienced prosthetist or orthotist…it may be problematic for you to let go of the craft of yours and go on to this method alone. You don’t want to go away from the successes you’ve made as an orthotist and the skills you’ve learned. Your hand skills and experience are utilized to correct that cast. Scanning a corrected cast then is optimal for this practitioner base. But if you have a large database that was out there, you could apply that to the patient scenario, and it predicts the corrections needed to be close enough, especially for someone who has less experience. Manufacturers such as Spinal Tech, Boston Brace, Atlantic Rim Brace Manufacturing, etc. have a database, and they can do a lot of predictive stuff. There are cases where it doesn’t work, but a lot of cases where they work quite well. For someone who doesn’t have the years of experience that another practitioner has, this data-driven method might be the way to go.”
In addition, there may be times where you can combine casting and scanning. “On the prosthetics side we’re doing 90 percent scanning over a limb,” says Joe Fairley, MPO, MS, CPO. “Especially for BK prosthetics it’s a lot easier to scan over the limb, as long as you take note of any bony anatomy you need to stay away from. For AK, where you want to capture the ischium, take a cast of just the brim section, scan the rest of the limb and inside of the brim, and merge the two in CAD. You get the best of both worlds.”
Incorporating new techniques and technology does not mean abandoning your experience and expertise but comes down to making a judgement call about what method will produce the best result for patients. As Derick Schmidt, MPO, CPO, says, “To me that becomes a question of mindset, and it’s the role of our clinical expertise and why we can’t just hand everything over to someone with a scanner. If you start looking at these digital tools as a shortcut to a delivery or device, you’ll find the shortcut—it’s there, but at what cost? But if you look at the digital tools as a way to improve patient outcomes and efficiency, it’s there too. There are benefits to be had, but we still have to do what we’re trained to do.”
We Are Committed to Scan. Now What?
If scanning a cast is chosen, how should we scan it?
By scanning the outside of a cast and then making a global reduction to account for the thickness of the cast, the actual shape of the limb can be captured, but there is some error due to the near impossibility of a completely uniform thickness. “Depending on the number of wraps you add to the cast, if you as the practitioner are good at making sure the number of wraps is consistent, you can do a reduction/offset for the thickness of the wraps,” Erenstone says. “On the flip side, in an AFO in which it can be difficult to get the dorsal surface at the ankle bend the same thickness as the rest of the cast, you’re going to end up with an error with that reduction. Your calcaneus will be too small/narrow. That’s not a great method, even though it can be used.”
Some manufacturers such as Cascade DAFO require caliper thickness measurements when scanning a negative cast of the first metatarsal head, just distal to the medial malleolus, and then posterior calf, which may help with this offset error.
One of the challenges clinicians encounter is that it is very difficult to scan the inside of a cast, since most scanners cannot capture a concavity that may be tucked under a prominence. With specific limb shapes, like a conical limb, it may be possible to scan from the top down. However, with bulbous limb shapes or AFOs, this is usually not possible due to the limitation the scanner runs into trying to see below and around these shapes or the transition from the ankle to the foot. One option is to split the cast in half, make markers on both sides, scan both halves, and digitally put them together. This method requires the software capability and the user’s skill to digitally stitch the two sides together, and it is very time consuming. Another method is to use a 3D scanner that can be dropped into the cast, scanning as it goes down. This has been used in fields such as dentistry but not widely in O&P. “This is one of the biggest bottlenecks [in digital manufacturing and workflow] because there isn’t a good option,” Erenstone says. “There needs to be a technological solution to this problem, an optical scanner with a short focal length, which can be done, because it has been done all the time in dental.”
Where to Begin
So how do you begin to implement CAD/CAM and scanning technology in clinical practice?
“Start small, start with scanning,” says Schmidt. “Once you get a good scan, you can now send it to someone else or learn the next step. Learn to get a good scan—it takes practice. It’s lighting, environment, how far you are from it, how fast you move. Start there. Then learning the CAD mods is the next step.” He also advises clinics to start small with their investment. “If you learn the skills, you can use free software and $500 printers.”
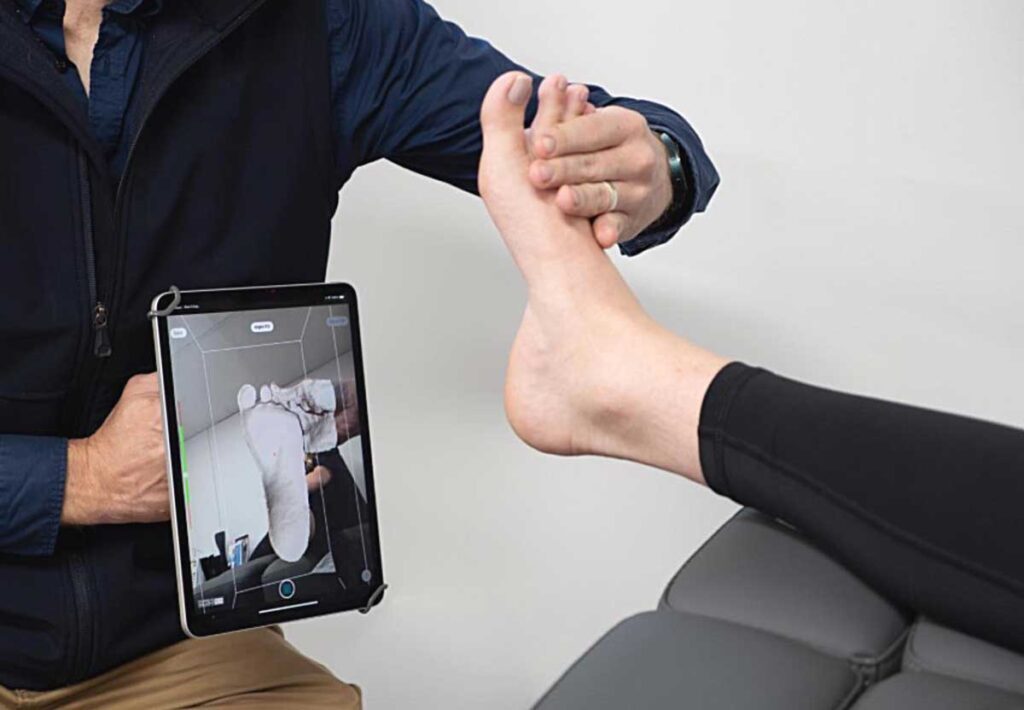
In terms of types of scanners, Erenstone says, “What serves our patients the best is the fastest, most convenient way to get the most appropriate information—we don’t need huge accuracy in the scan if we don’t need to use huge accuracy.” With burn mask orthoses sometimes you need a high level of accuracy in the central region of the face, but an AFO or TLSO typically does not need to be accurate to a fraction of a millimeter in circumference. The authors have had success with iPhone scanning technologies such as the Comb Scanner app (Figure 4).
Erenstone continues, “If you have a patient that can only be in a certain position for a short period of time, the best thing is to scan quickly. As long as that fast scan is accurate enough, that’s the best thing for the patient.”
Improved Workflow and Advantages of Scans
Recent software development has led to programs tailored specifically for O&P practitioners. Outside of the difficulty scanning the inside of a cast, some of the technology has lacked an end-to-end workflow that is simple and relatable to traditional clinical modifications or required learning CAD, which requires a significant time investment and might not be intuitive for practitioners who have learned plaster modifications. These new programs and their specific tools allow practitioners to learn software that only covers what is needed to modify the mold, as if doing so physically, instead of having to go to a separate program to study software that does everything. Being gadget-focused, as most in this field are, it’s common for us to have a lot of tools around the house that we will never need. But in the shop, we have the essentials only, and that is what the software specific to O&P allows for in CAD. There is also always the option to partner with a fabrication lab that does CAD modifications, just as if you were sending a physical mold to a central fab.
The process of traditional fabrication is time intensive and difficult and relies on a fully staffed technician team, but by using this technology, O&P practices can streamline the process and do things more quickly, and often, in the case of 3D printing, around the clock. A colleague once likened the 3D printer in her practice to storybook characters, “The elves come to work, and when I come in in the morning there is a socket on the plate printed overnight. It’s magic!”
Additionally, scans allow for devices to be duplicated exactly if they need to be remade. If an adjustment is needed before refabrication, that can be done quickly on the computer instead of having to recast or pull out an old plaster model. Instead of a warehouse of old plaster molds sitting around and being destroyed due to physical space limitations, there can be an endless digital library. Once we find a good method to scan the inside of a cast or socket, a prosthetist could fit a check socket, make all of the in-person adjustments there with the patient (heating and flaring, adding pads, etc.), and then scan the modified socket and have the final version, instead of having to repour or make all the adjustments in CAD.
Having scans can also improve the patient’s treatment over time. Having the ability to store digital scans could lead to tracking limb shape changes over time, moving toward more standardization and implementation of outcomes-based treatment. Fairley points out that this will eventually be a necessity. “The more that we become outcomes based, and our reimbursement depends on it, in order to have all the justifications needed, they’re going to require 3D scans. These are the things we need to think about as clinicians to be prepared for and aware of how our patients’ limbs are changing.” With a large enough database of information, we could begin to identify certain criteria that require a particular modification, thus leading to models of treatment plans based on the data a patient presents with.
There is also potential for new options in the cosmesis of the devices we’re providing. “We have more options with 3D printed; you can do a textured pattern, with different thicknesses and an embossed pattern,” Erenstone says. “You could do something printed and then do a wrap to get a really cool pattern on it. There are definitely easy solutions to the cosmesis.” 3D printing a pattern such as a multicolor unicorn, however, requires a more expensive multicolor printer. Once again, the options for what could be done with the technology today are outpacing what is currently being done.
Changing Workforce Trends
3D printing as a trend may also be a response to a smaller pool of technicians. In a 3D printing session at an Academy meeting last year, a colleague said he was being forced toward 3D printing because his area had lost technicians to places like Amazon warehouses, and he needed to use other means of fabrication for the practice to survive.
As new technology and techniques make their way into fabrication, we may see the idea of a digital technician become a reality. These digital technicians would be well versed in CAD modifications and do the work digitally that was done manually in traditional fabrication. These digital technicians would work alongside practitioners, freeing them to focus on patient care without having to invest time into learning CAD, while still allowing the practice to incorporate the benefits of manufacturing with scanning and CAD technology. However, it is necessary to consider the education needed to support it.
“You only need to teach [a digital technician] some clinical things, not all clinical things. We’re not losing techs by changing them into digital technicians,” Fairley says. “There’s a shift in mentality between who we’re hiring and why we’re hiring them. I love the hands-on aspect and the craftsmanship style, and there will always be a place for it, but the more we shift to digital, the less and less we’re going to be using these manual techniques that aren’t repeatable. It’s all about the way we’re going to be able to design things and match the right materials with that design process.”
The conversation mentioned in the beginning of the article spurred Keith to ask recent residents how much scanning, CAD software, and 3D printing they had learned in school. The answers ranged from zero to very little. As we see scanning and CAD evolve and grow more mainstream in O&P, we may also see these techniques make their way into the curriculum.
In speaking to a recent dental school graduate, Keith found a similar trend—the student had an introduction to scanning and has taken multiple weekend courses post-graduation to increase his knowledge base and skills in the more advanced techniques. The school sets the foundation for practicing dentistry; beyond that, what dentists learn depends on what procedures and techniques they want to do and their level of expertise in it. The MOD Institute, for instance, has weekend courses for dentists wanting to expand their skillsets. It seems an investment in time and continuing ed courses is what is driving the dental industry to more advanced techniques in scanning and printing.
In O&P, we are starting to see similar models. For example, an article in The O&P EDGE cites that Fairley has educated 15 new 3D-printing adopters over the last two years, beginning with two days of onsite instruction.2
It appears that O&P has the ability to further the levels and means of measuring and fabricating devices with another tool available to practitioners. Some in the future will cast only, some will scan only, some will be 3D printing, and most will use a combination of all three. Some may team up with central fabrication by sending molds, digital files, or both. Some may team up with digital partners or hire digital technicians. The authors believe that as barriers to entry have lessened, O&P needs new pathways through continuing education to foster digital adoption. Formal training really won’t be necessary to dabble in these advanced topics and techniques, but to go to the next level of usage and expertise more continuing education pathways will be essential.
Keith M. Smith, CO/L, FAAOP, is a practitioner with the Orthotic and Prosthetic Lab, Missouri. He can be contacted at keithorth@sbcglobal.net.
Elizabeth Johnsen, MSOP, is a resident with the Orthotic and Prosthetic Lab. She can be reached at ejohnsen@oandplabinc.com.