Researchers are advancing a new generation of fully customizable prosthetic sockets by integrating artificial intelligence (AI) with 3D printing — a development that could significantly improve comfort, biomechanics and long-term outcomes for people with limb loss.
Traditional socket fabrication typically relies on casts or digital scans to capture limb shape and volume. While these methods provide precise dimensional data, they generally don’t account for how pressure and force distributions vary across an individual’s residual limb during everyday activities such as standing, walking or changing direction.
In a recent study published in Biosensors and Bioelectronics, researchers at Simon Fraser University developed an innovative workflow that begins with real-world pressure mapping and ends with an AI-optimised 3D printed socket that is lighter, more breathable and more responsive to individual biomechanics.
From Pressure Mapping to Personalized Design
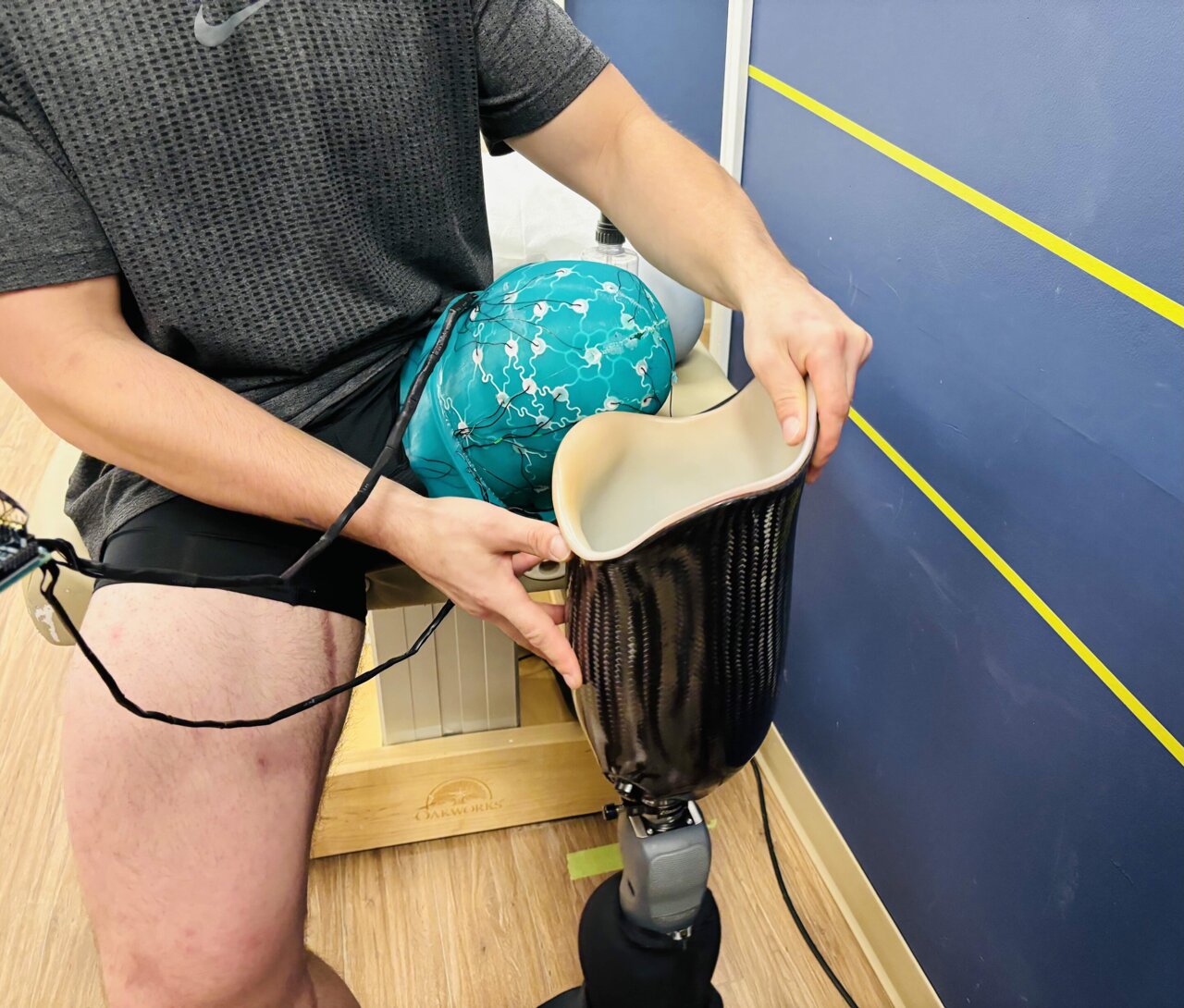
At the heart of the new approach is a miniature pressure-sensing liner worn inside a temporary socket. The liner is embedded with a network of sensors that detect localized pressure and force patterns as the wearer:
- Stands
- Walks on flat ground
- Descends inclines
- Shifts balance in daily postures
These dynamic data points are then processed by AI software that interprets the pressure distribution and generates a customized socket design incorporating a lattice-style internal structure — a repeating 3D pattern inspired by natural geometries such as bone trabeculae or honeycomb formations.
Once the design is complete, it is 3D printed using lightweight materials that can deliver improved energy absorption and comfort compared to traditional solid-infill sockets.
Measurable Performance Gains
In laboratory testing, the lattice-structured sockets demonstrated remarkable mechanical benefits:
- Up to 1,600% greater energy absorption while standing
- Up to 1,290% greater energy absorption during walking
Relative to conventional solid-infill sockets tested under similar conditions, these results suggest that optimized internal structures can significantly cushion impact forces and reduce peak pressure points — two factors closely linked with common socket-related complications such as skin irritation, pain and instability.
For clinicians, improved energy distribution and reduced peak stresses may translate into:
- Better ambulation comfort
- Lower risk of skin ulceration
- Enhanced gait stability
- Reduced compensatory movement patterns
These outcomes align with broader clinical goals in prosthetic practice and rehabilitation.
Bridging Research and Clinical Practice
Clinical partners such as Hodgson Group Orthotics and Prosthetics played a role in evaluating the technology and interpreting how data-informed design could impact everyday use. Practitioners involved in the study noted that AI-driven customization offers a new dimension of objective insight that supplements — and in some areas, extends — traditional clinical judgement.
One prosthetist described how this data-rich design process provides a more nuanced understanding of limb–socket interaction, potentially reducing the need for repeated adjustments and remakes — a persistent challenge in prosthetic service delivery.
Implications for the O&P Community
For prosthetists, orthotists and rehabilitation teams operating in both high-resource and lower-resource settings, the evolving integration of AI and additive manufacturing suggests several practical opportunities:
- Enhanced precision in socket design tailored to individual biomechanics
- Reduced cycle time for iterative fittings, thanks to digital feedback loops
- Potential cost benefits through fewer remakes and improved patient satisfaction
- Expanded access to advanced customization where local fabrication is available
Research trends like this also dovetail with broader industry movements toward digital workflows, including 3D scanning, CAD-based designs and networked fabrication systems.
Looking Ahead
While 3D printing and AI are not new to the prosthetics field, their combined use in utilising real-world pressure data for optimized socket structures represents a step forward in personalization and patient-centred design. As additive manufacturing technology becomes more widespread and computational modelling tools more sophisticated, such hybrid approaches may one day become part of mainstream prosthetic practice.
The study highlights the promise of data-driven design — offering clinicians and patients a path toward sockets that are not only anatomically accurate, but also responsive to the unique mechanical demands of everyday life.