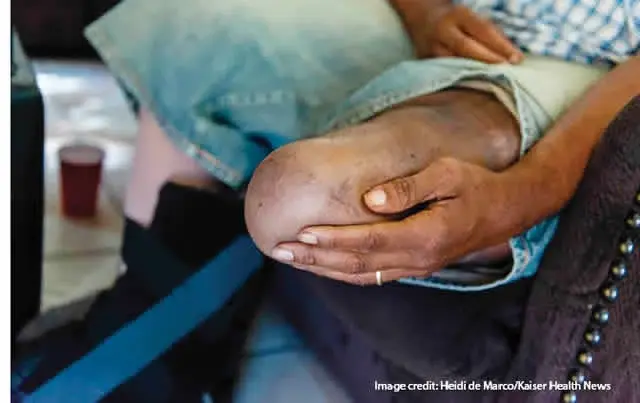
Senior Nigerian medical specialists are warning that diabetes has become one of the country’s leading causes of limb loss, with about 60% of limb amputations now linked to the disease, according to a report published by PUNCH Healthwise on April 5, 2026.
The concern is rooted in the growing burden of diabetic foot complications, especially ulcers, infection, gangrene, nerve damage, and poor blood circulation in the lower limbs. PUNCH Healthwise says specialists believe these complications are now driving a large share of amputations in Nigerian hospitals, particularly when patients present late for treatment.
According to the report, clinicians say the legs and feet are the most commonly affected areas, reflecting the typical pattern of diabetic limb loss. The article notes that amputations linked to diabetes may now exceed trauma-related amputations in some centres, highlighting how strongly chronic disease is shaping surgical and rehabilitation demand.
For IMEA CPO readers, this is the key issue. Nigeria’s amputation burden is not only a trauma story. It is increasingly a diabetic foot and chronic disease story as well. That has major implications for orthotics, prosthetics, podiatry, wound care, and rehabilitation, because it shifts attention toward earlier prevention, offloading, protective footwear, custom insole use, wound referral, and post-amputation support. This is an inference based on the specialist warnings reported by PUNCH Healthwise.
The article also points to a familiar systems problem: late presentation. Patients often reach hospital only after wounds have worsened significantly, reducing the chance of limb salvage and increasing the likelihood of partial foot or major lower-limb amputation. In practical terms, that means many cases that might have been managed earlier through better glucose control, regular foot checks, proper footwear, and earlier wound care are instead reaching advanced stages.
That matters because once diabetic foot disease progresses to serious infection or gangrene, the consequences extend well beyond surgery. Patients may require longer hospital stays, rehabilitation, prosthetic fitting, mobility aids, repeat follow-up, and wider social support. In lower-resource settings, the cost to families and health systems can be severe. This is an inference, but it follows directly from the clinical pathway described in the PUNCH Healthwise report.
The story also highlights a broader evidence gap. Nigerian specialists told PUNCH Healthwise that the country still lacks a strong national amputation database, which makes it harder to measure the full scale of diabetes-related limb loss across all regions. Even so, the consistency of the observations from specialists suggests the problem is already highly visible in day-to-day clinical practice.
Older published Nigerian evidence gives useful context here. A retrospective study from a tertiary hospital in northwestern Nigeria found that diabetic foot gangrene accounted for 21% of major amputations between 2008 and 2014, second only to trauma in that centre. That earlier figure predates the latest specialist warnings, but it shows that diabetes-related amputation has been a serious issue in Nigeria for years and may now be worsening.
Why this matters
The strongest takeaway is that diabetes in Nigeria is no longer only an internal medicine issue. It is increasingly a limb-loss and rehabilitation issue too. For the O&P sector, that means the response cannot begin only after amputation. It also has to include stronger diabetic foot prevention pathways, patient education, earlier screening, offloading, wound management, and practical lower-limb protection strategies designed to reduce avoidable limb loss before it happens. This conclusion is an inference based on the reporting and supporting Nigerian amputation literature.