A recent article from The Borgen Project has highlighted the role of Amparo’s Confidence Socket technology in improving prosthetic access for Kenyan amputees, particularly in communities where conventional prosthetic services may be difficult to reach. The article frames the technology as a potential response to a wider challenge across Kenya: many people with mobility-related disabilities continue to face barriers linked to cost, geography, public health infrastructure and limited access to specialist rehabilitation services.
For prosthetics and orthotics professionals, the Kenya example is important because it shows how socket design, fitting speed, portability and follow-up capacity can directly affect whether amputees receive a usable prosthesis at all. In lower-resource environments, the socket is not just a technical component. It is often the difference between a prosthesis that can be delivered, adjusted and used — and one that remains out of reach.
Why Kenya’s Amputee Population Needs Better Prosthetic Access
Kenya’s need for prosthetic and orthotic services is shaped by a mix of trauma, diabetes, infection, congenital limb difference and wider disability-related barriers. The Borgen Project article notes that mobility-related disability is a major issue in Kenya and that many people with disabilities live in rural areas, where access to adapted public services and specialist rehabilitation can be limited.
Research on limb amputation at a Kenyan rural hospital found trauma to be the leading cause of amputation in that setting, accounting for 35.7% of cases, followed by congenital defects, infection and tumours. Diabetes-related vascular disease also represented a significant share of dysvascular amputations.
Diabetes is an increasingly important factor for prosthetic and orthotic planning in Kenya. The International Diabetes Federation previously estimated that more than 550,000 adults were living with diabetes in Kenya, with more than one in three undiagnosed at the time of reporting. More recent IDF figures for 2025 estimate around 813,300 adults living with diabetes in the country.
For O&P services, this means Kenya requires both prosthetic access and stronger preventive pathways. Early diabetes screening, diabetic foot care, appropriate footwear, foot orthoses, wound care referral and timely rehabilitation can all reduce the long-term burden of avoidable amputation.
What Is the Amparo Confidence Socket?
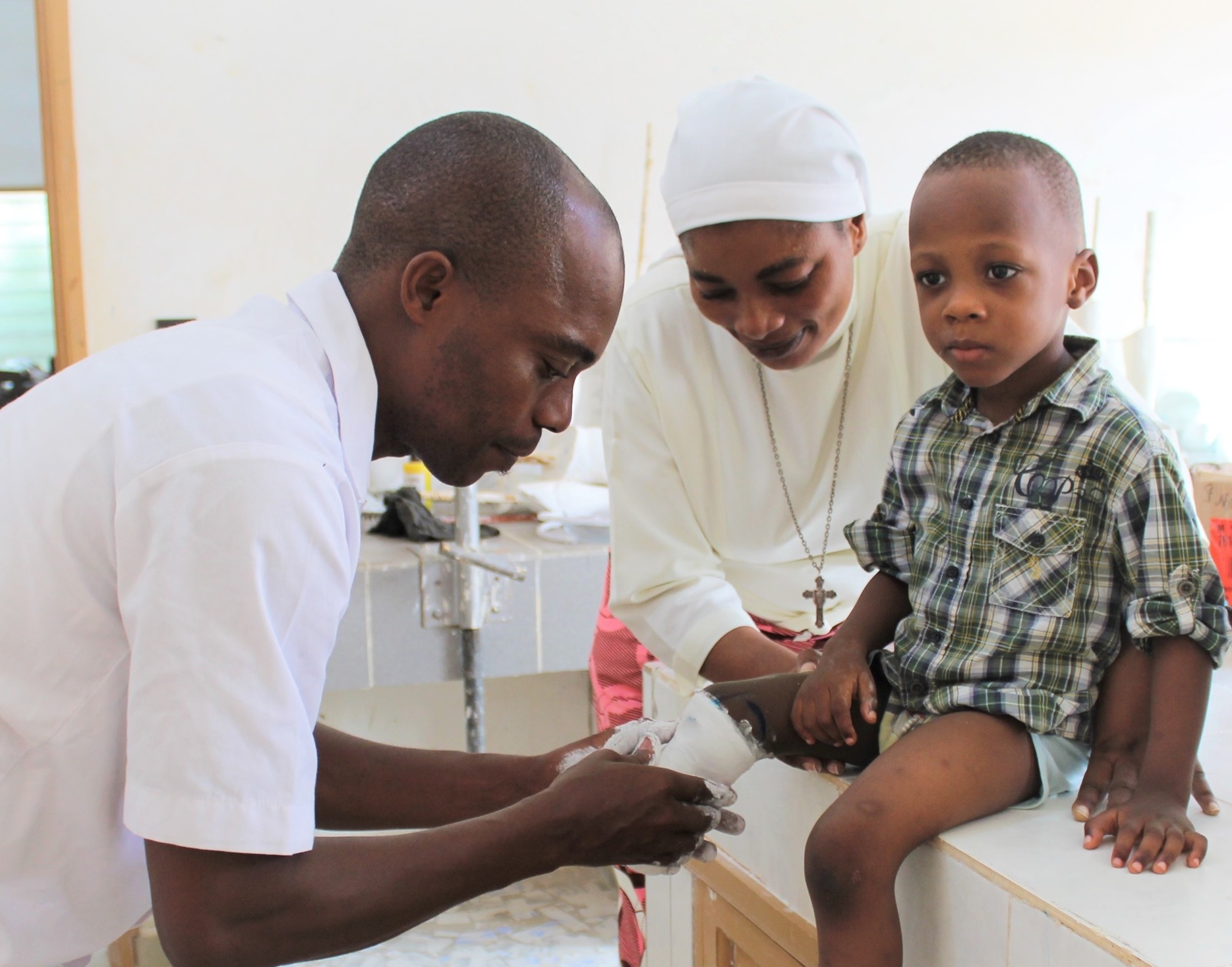
The Amparo Confidence Socket is a thermoplastic below-knee prosthetic socket system designed to simplify and speed up the fitting process. Unlike conventional socket fabrication, which may require plaster casting, specialised workshop equipment and multiple appointments, the Amparo approach uses a direct-fit model that can be moulded and adjusted more rapidly.
The Global Disability Innovation Hub describes the technology as easier and faster to fit than many traditional prosthetic manufacturing methods, with the added advantage that it can be remoulded when adjustments are needed. The system was also designed with field use and remote-area application in mind, making it relevant for countries where patients may live far from central prosthetic workshops.
This is particularly relevant in Kenya, where many amputees may face long travel distances, transport costs and limited access to repeated follow-up appointments. A socket that can be fitted more quickly and adjusted closer to the patient has the potential to improve access, especially when combined with trained clinicians and technicians.
Evidence from Kenya
A study evaluating a thermoplastic socket in Kenya examined the use of the Confidence Socket and its impact on functional mobility, comfort, quality of life and user satisfaction. The research concluded that the Amparo Confidence Socket could be a viable way to improve access to appropriate prosthetic care in Kenya, while also noting that comfort and long-term use require further attention.
This balance is important. Faster fitting and easier deployment are valuable, but prosthetic success depends on much more than initial delivery. Comfort, pressure distribution, suspension, residual limb changes, gait training, repair services and user follow-up remain essential. A socket solution that improves access must still meet clinical standards and support long-term function.
Why This Matters for O&P in Africa
The Kenyan example reflects a wider issue across Africa and other low- and middle-income settings. Traditional prosthetic care often depends on skilled personnel, imported components, workshop infrastructure and multiple patient visits. These requirements can make care expensive and difficult to scale.
Innovations such as the Amparo Confidence Socket may help address part of that challenge by reducing fabrication complexity and improving portability. However, they should not be seen as a replacement for professional O&P services. Instead, they should be understood as one possible tool within a broader rehabilitation system.
For best results, technologies like this need to be integrated with:
- Clinical assessment by trained prosthetists and rehabilitation teams
- Appropriate patient selection
- Gait training and physiotherapy
- Follow-up and socket adjustment
- Local repair and maintenance capacity
- Clear referral pathways for complex cases
- Long-term outcome tracking
In Kenya and across the IMEA region, the question is not whether innovation is needed. It clearly is. The more important question is how new technologies can be introduced responsibly, affordably and sustainably.
The Role of Local Capacity
Kenya has a growing rehabilitation and assistive technology ecosystem, including public hospitals, private clinics, NGO-supported services, academic institutions and innovation partners. But service access remains uneven, especially for rural patients and low-income households.
For prosthetic socket technologies to have lasting impact, local capacity must remain central. This means training Kenyan prosthetists, orthotists, technicians and physiotherapists to assess, fit, modify and follow up patients using new systems. It also means ensuring that supply chains, spare parts and repair processes are available after the initial fitting.
Technology can accelerate service delivery, but only local professional capacity can sustain it.
A Broader Lesson for the Region
The Amparo Confidence Socket story in Kenya is a useful case study for the wider O&P sector. It demonstrates how design choices can influence access. A socket that is portable, remouldable and faster to fit may be highly relevant in rural and resource-constrained settings.
At the same time, the Kenyan experience also reinforces the importance of evidence. New prosthetic technologies should be evaluated not only for fitting speed, but also for comfort, mobility outcomes, durability, user satisfaction, affordability and long-term follow-up.
For amputees, the goal is not simply to receive a prosthesis. The goal is to walk safely, return to school or work, participate in family and community life, and maintain independence over time.
Outlook
Kenya’s experience with the Amparo Confidence Socket points toward an important future for prosthetic care in Africa: faster, more mobile, more adaptable and more patient-centred service delivery.
The technology may not solve every challenge facing Kenyan amputees, but it highlights a practical direction for the sector. When combined with trained professionals, strong rehabilitation pathways and sustainable follow-up, innovative socket systems can help reduce the distance between need and access.
For the IMEA O&P community, the message is clear: prosthetic innovation must be judged by its ability to reach real patients in real-world settings. In Kenya, that means solutions that are clinically sound, locally maintainable, affordable and designed around the daily lives of amputees.
- Original article: The Borgen Project – Amparo Confidence Sockets and Kenyan Amputees
- Amparo Prosthetics
- Amparo Confidence Socket information
- Global Disability Innovation Hub – Changing Prosthetic Service Delivery with Amparo
- Evaluation of a thermoplastic socket in Kenya
- International Diabetes Federation – Kenya
- Research on limb amputation patterns in a Kenyan rural hospital
- WHO Rehabilitation 2030 Initiative
- International Society for Prosthetics and Orthotics