A new generation of paediatric orthotic research is showing how digital tools could transform brace design for children with cerebral palsy — and it is being helped forward by an Iranian-trained clinician now working in New Zealand. According to the University of Auckland, Sara Chami, who previously worked as a clinical orthotist in Tehran, is developing a more personalised brace system that combines weight-bearing 3D scanning, modular design and activity-specific tuning to improve comfort, function and wearability for children with cerebral palsy.
The problem she is addressing is familiar across many rehabilitation systems. Conventional ankle-foot braces can be bulky, rigid and uncomfortable, and when children do not tolerate them well, adherence drops. The University of Auckland notes that around half of children with cerebral palsy need ankle-foot braces to support walking and reduce the risk of contracture, yet traditional fabrication remains labour-intensive and can depend heavily on clinician skill, plaster casting and lengthy production pathways.
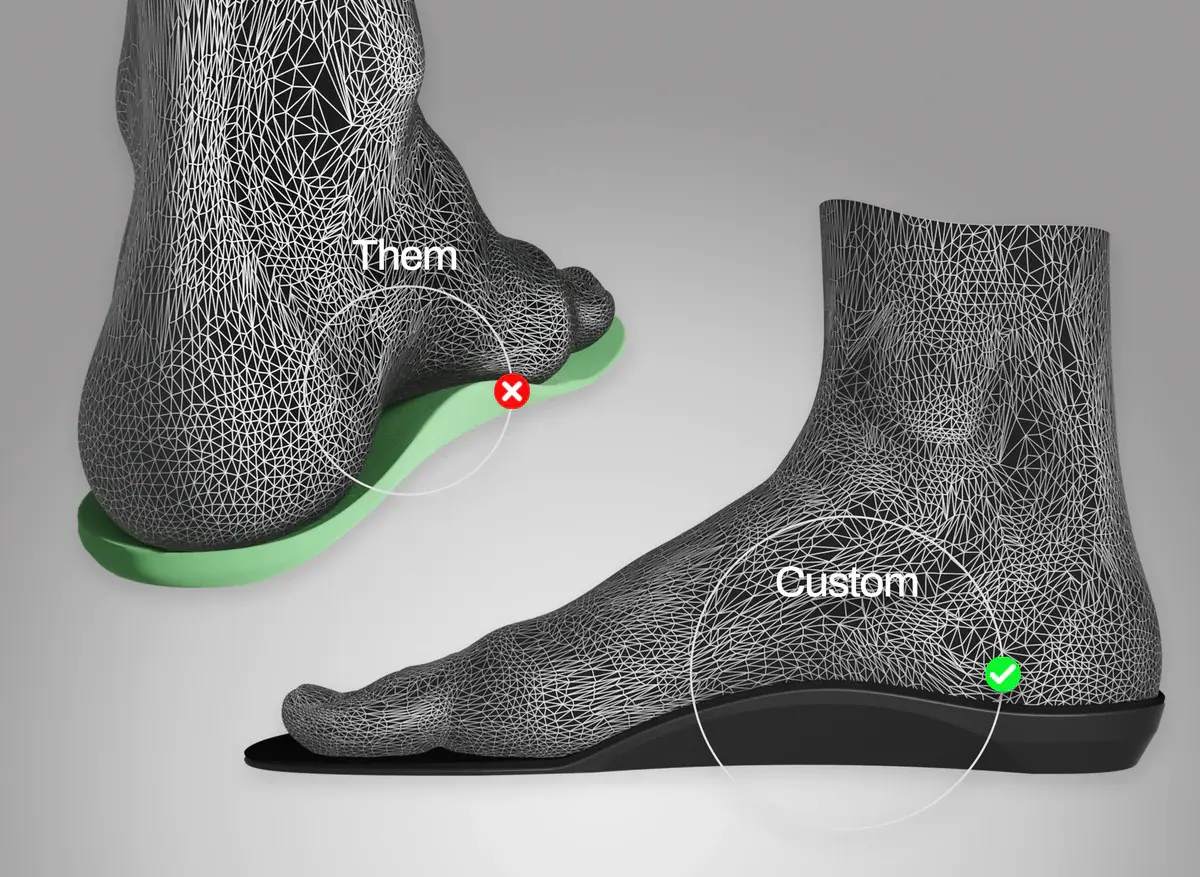
Chami’s work aims to change that model. Her brace concept begins with a digital, weight-bearing 3D scan of the foot and ankle, which is used to create a patient-specific orthotic design. The university reports that the brace is modular, with an insole, a below-knee section and interchangeable carbon-fibre rods that allow stiffness to be adjusted according to the child’s needs and activity. That means support could potentially be tuned for walking, play, cycling or other daily movement demands rather than forcing one rigid solution onto every task.
What makes the project especially interesting for the global O&P sector is its attempt to personalise stiffness, not just fit. Chami is using a human-in-the-loop optimisation approach in which children trial the brace under different conditions while gait and ankle performance are measured. The goal is to identify the most appropriate stiffness profile for each child and then adapt the brace accordingly. This moves orthotic practice closer to data-informed functional tuning rather than shape-based fabrication alone.
For IMEA CPO readers, there is a second story here as well: the importance of diaspora expertise. Chami’s journey from clinical orthotic work in Tehran to advanced research at the Auckland Bioengineering Institute reflects a wider pattern seen across healthcare and rehabilitation. Diaspora CPOs often carry practical experience from one health system into another, linking clinical realities, engineering innovation and new methods of service delivery. In this case, an Iranian-trained orthotist is helping push forward a brace model that could eventually benefit not only children with cerebral palsy, but also wider patient groups such as people recovering from stroke, as the University of Auckland notes.
That has broader significance for the profession. Iranian diaspora clinicians, prosthetists and orthotists working across Europe, Oceania, North America and the Middle East can play an important role in global O&P development. They often bring strong technical training, direct experience of resource constraints, and a practical mindset around adaptation and problem-solving. When those strengths are combined with access to research infrastructure, digital manufacturing and interdisciplinary teams abroad, the result can be highly relevant innovation for both advanced and emerging markets. This is an inference from Chami’s professional path and the kind of translational research now being reported around her work.
There is also a lesson here for the IMEA region. Better paediatric bracing will not come only from importing finished devices. It is more likely to come from building systems that combine clinician insight, digital capture, functional testing and flexible fabrication. Projects like this point toward a future in which CPOs are not only device fitters, but also data-enabled movement specialists shaping more adaptive orthotic care.
At its heart, this is still a very human story. The University of Auckland quotes Chami’s vision simply: that families can finally say they have found a brace their child is happy to wear. In paediatric orthotics, that may be one of the most important outcomes of all.