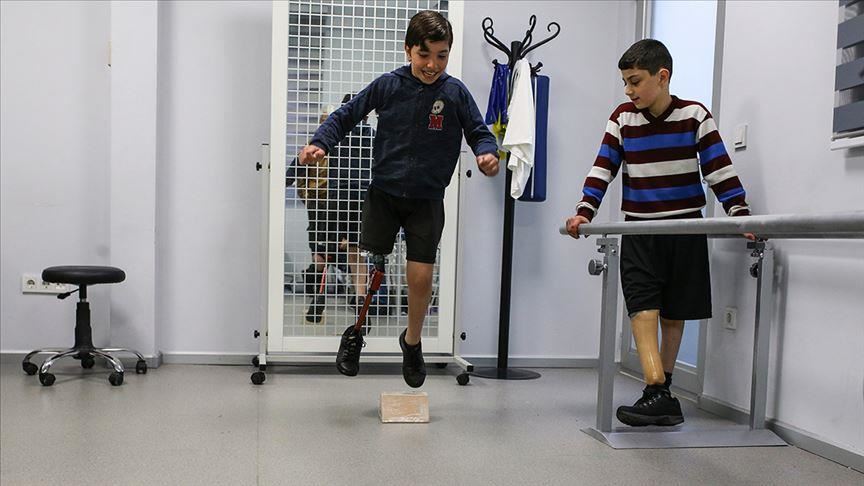
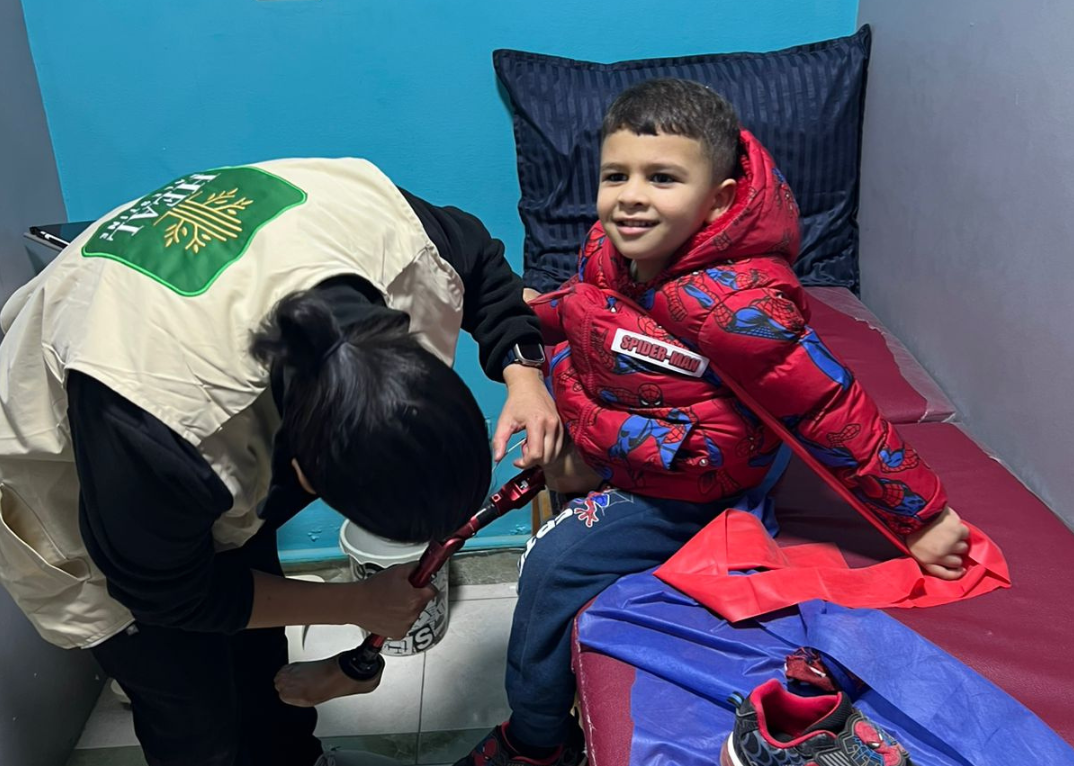
A new study protocol published in PLOS ONE sets out an ambitious goal for pediatric prosthetics research: to listen more directly and more effectively to children living with lower limb loss, rather than relying mainly on adult interpretations of their needs. The paper, published on 31 October 2024, describes the rationale, design, and delivery plan for a globally applicable research toolkit focused on prosthetic user needs, quality of life, pain, and physical function in children.
The authors argue that rehabilitation after childhood lower limb loss is especially complex because it is shaped not only by the child’s physical condition, but also by caregivers, clinicians, service systems, and the wider environment. Yet despite the central importance of user input in prosthetic innovation, children are often excluded from direct research participation or are not engaged in ways that suit their age and development. The protocol was designed specifically to address that gap.
The project looks at children in three contrasting settings: Cambodia, the Gaza Strip, and the United Kingdom, with the aim of building a more internationally relevant understanding of life with lower limb loss. The authors say a literature review showed that existing tools were not well suited to identifying the specific requirements of pediatric prosthetic users, which led them to create new stakeholder-specific interview guides for the child, caregiver, and prosthetist.
One of the most important aspects of the protocol is that the child’s research guide was deliberately designed around enjoyment and engagement, including the use of card games and activities to help children participate more comfortably and meaningfully. The toolkit was then reviewed by a panel of experts in pediatric limb loss and mental health, and combined with existing validated measures covering quality of life, pain, and mobility. According to the paper, the full toolkit was successfully piloted with five children, their families, and two prosthetists.
The rationale for this work is striking. The paper notes that an estimated 64% of people living with amputation worldwide were in low- and middle-income countries in 2020, and that children carry a large share of the disability burden. It also points out that 420 million children were living in conflict-affected areas in 2017, where traumatic injuries, including lower limb loss, are common. In that context, the authors argue that pediatric prosthetic research has too often been dominated by adult priorities or by scaled-down adult solutions that do not adequately reflect children’s unique physical, emotional, and developmental needs.
The paper makes another important point for the O&P profession: the child is only one part of the prosthetic user chain. Parents and caregivers often understand the child’s daily challenges across school, self-care, community participation, and family life, while clinicians bring insight into fitting, supply, rehabilitation, and component use. The authors say relatively few published studies have incorporated the full chain of child, parent, and clinician in a structured way, and that this has slowed more effective design innovation.
That matters because many existing studies either treat the prosthetic limb as a single system or focus only on narrow themes such as cosmesis or participation. The authors argue that this leaves designers and clinicians with too little detail about how individual prosthetic components affect a child’s experience. They also note that many studies focus on only one amputation level, such as transtibial loss, making it harder to understand where needs differ across levels of limb loss.
For the wider rehabilitation field, this protocol is significant because it is not simply a call for more research. It is a call for better methods. By setting out a child-centered, ethically reviewed, internationally applicable toolkit, the authors are trying to create a more practical way to capture evidence that can inform both clinical care and future design solutions. The study implementation period is described as running from January 2023 to December 2025, with results intended for dissemination through conferences and peer-reviewed publications.
For IMEA CPO readers, the relevance is especially strong. Many children with limb loss in emerging markets and conflict-affected settings still face limited access to appropriate pediatric prosthetic services, and their needs are often filtered through adult assumptions. A research model that actively centers the child’s own experience could help reshape how pediatric prosthetic care is assessed, delivered, and improved, particularly in lower-resource contexts. That final point is an inference based on the authors’ stated rationale and the inclusion of settings such as Cambodia and Gaza alongside the UK.
Ultimately, this PLOS ONE paper is a protocol rather than an outcomes paper, so it does not yet provide final findings on what children need most. But it does something important nonetheless: it sets up a structure for listening more carefully to children with lower limb loss, and for using that evidence to improve prosthetic design, rehabilitation, and quality of life in a way that is more globally relevant and more ethically grounded.