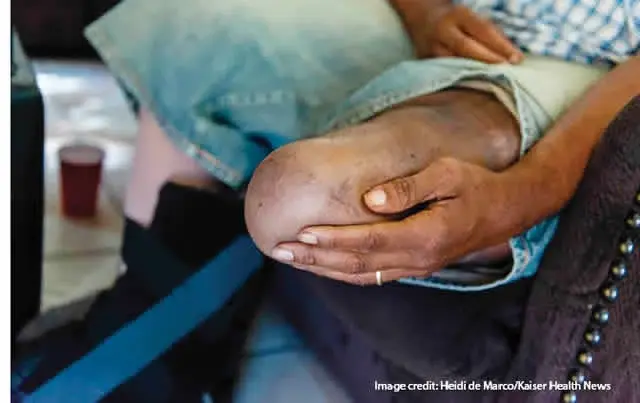
Ugandan clinicians are warning that diabetic amputations are increasing as more patients present late with advanced foot complications, often after ulcers, infection, and gangrene have already taken hold. In New Vision’s April 2026 report, diabetes specialist Dr Silver Bahendeka said diabetes damages blood vessels, with those in the legs especially vulnerable, while the case story at the centre of the article illustrated the heavy financial and clinical burden that delayed care can create.
The broader diabetes burden in Uganda is also rising. The IDF Atlas estimates that 369,100 adults aged 20 to 79 were living with diabetes in Uganda in 2024, while the IDF member page for Uganda puts adult prevalence at 2.2%. WHO Africa has also said diabetes is one of the leading causes of non-traumatic lower-limb amputation in Uganda and noted that many Ugandans with diabetes remain undiagnosed or untreated until complications become difficult to manage.
That combination helps explain why limb loss is becoming a bigger issue. When diabetes is poorly controlled, high blood sugar can damage nerves and blood vessels over time. Loss of sensation means minor injuries may go unnoticed, while poor circulation makes wounds slower to heal and more likely to become infected. According to WHO Africa, diabetes in Uganda is also tied to serious complications affecting vision, kidneys, blood vessels, and lower limbs, reinforcing the need to view diabetic foot disease as both a medical and rehabilitation challenge.
The New Vision article points to late presentation as a major part of the problem. Patients frequently arrive for treatment when disease has already advanced, making limb salvage harder and increasing the likelihood of partial foot or major lower-limb amputation. That pattern is consistent with WHO Africa’s warning that a large share of Ugandans with diabetes are not aware of their condition or are not on treatment, so they first reach the health system with complications that are more difficult and more expensive to treat.
Diet and lifestyle pressures are part of the wider picture too. A separate New Vision report on diabetes in Uganda cited Ministry of Health-linked figures showing that diabetes prevalence among Ugandans aged 40 and above had risen from 1.4% in 2014 to 3.3% more recently, while a Makerere-linked study explored how entrenched dietary and social norms may be contributing to the country’s growing type 2 diabetes burden. The same report quoted clinicians warning that excess carbohydrate intake, obesity, and sedentary lifestyles are increasing risk.
For IMEA CPO readers, the story is important because it shows that diabetic limb loss is not only a surgical issue. It is also an orthotics, prosthetics, podiatry, wound-care, and rehabilitation issue. Rising amputations point to the need for much stronger pathways around screening, foot protection, offloading, early wound referral, custom insoles, protective footwear, patient education, and post-amputation rehabilitation. That conclusion is an inference from the reported rise in diabetic complications and the established role of diabetes in lower-limb amputation.
It also underlines the economic cost of delayed intervention. Once a patient progresses from neuropathy and ulceration to severe infection or gangrene, the burden shifts rapidly from prevention to surgery, inpatient care, mobility loss, rehabilitation, and long-term disability support. In lower-resource settings, that often means greater family financial pressure and a heavier load on already stretched health services. This is an inference, but it follows directly from the clinical pathway described in the reporting and from WHO’s framing of diabetes complications in Uganda.
Why this matters
The most important takeaway is that Uganda’s rise in diabetic amputations appears to be driven by a combination of growing diabetes prevalence, late diagnosis, delayed care, vascular and nerve damage, and limited early foot management. For the O&P and rehabilitation sector, that means the strongest response is not only better prosthetic care after limb loss, but much earlier diabetic foot intervention designed to stop avoidable amputations before they happen.