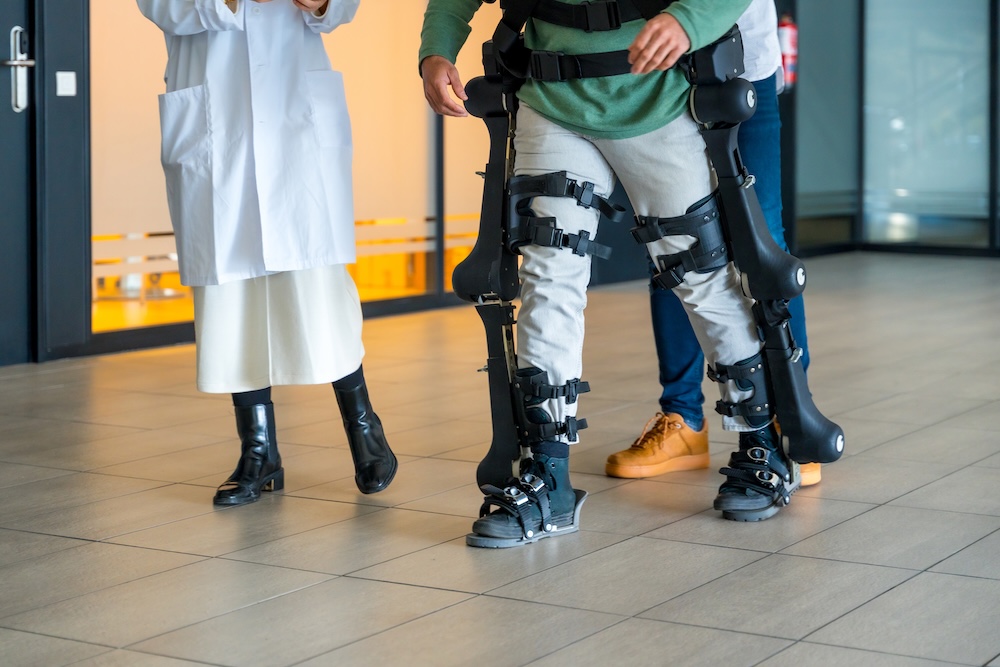
Brain-controlled exoskeleton technology could offer new hope for people living with spinal cord injury, as researchers continue to explore how brain-computer interfaces may help patients regain intentional movement and improve rehabilitation outcomes.
A report by NR Times highlights the potential of robotic exoskeletons that respond to brain signals, allowing users with severe paralysis to control assisted movement. The concept is part of a wider field of neuroprosthetics, where implanted or wearable sensors decode user intent and translate it into movement through robotics, stimulation systems or external devices.
One of the best-known examples came from a French research team in Grenoble, where a man with tetraplegia was able to walk using a four-limb robotic exoskeleton controlled by signals from his brain. The system used implanted wireless recorders positioned above the sensorimotor cortex, with decoded brain activity used to control the exoskeleton in real time. The work was published in The Lancet Neurology and was widely reported as an important proof-of-concept for brain-controlled mobility systems. Reuters coverage via the World Economic Forum described how the patient first trained with a computer avatar before progressing to the physical exoskeleton.
For spinal cord injury patients, the significance is not only the visual impact of standing or walking again. Exoskeleton-assisted rehabilitation may support weight-bearing, upright posture, stepping practice, circulation, cardiovascular conditioning, bowel and bladder health, psychological wellbeing and social participation. It can also give rehabilitation teams a structured way to deliver repetitive gait training, which is often difficult to achieve manually.
A recent systematic review and meta-analysis published in Systematic Reviews found that exoskeleton robotic training can significantly improve several motor-function measures in people with spinal cord injury, including the six-minute walk test, 10-metre walk test, Walking Index for Spinal Cord Injury, Timed Up and Go and lower-extremity motor scores. The review included 13 trials with 247 participants and found the greatest gains with medium training intensity, corresponding to around 1,000–2,000 cumulative minutes of training.
For CPOs, rehabilitation engineers and assistive technology teams, brain-controlled exoskeletons represent a convergence of several fields: orthotic bracing, robotics, neuroengineering, gait training, sensor technology, software, patient safety and long-term rehabilitation planning. Unlike conventional orthoses, these systems do not simply support weak or unstable joints. They actively interpret movement intent and provide powered assistance.
This creates both opportunity and caution. Brain-controlled exoskeletons remain complex, expensive and largely limited to research or specialised clinical environments. Many systems still require safety harnesses, extensive training, careful supervision and controlled settings. The French tetraplegia trial, for example, was described by researchers as a breakthrough but not yet a device ready for routine home use.
The immediate clinical relevance may therefore be rehabilitation rather than independent community mobility. For SCI patients, exoskeleton sessions can become part of a broader therapy programme alongside physiotherapy, wheelchair skills, pressure management, standing frames, orthotic assessment, functional electrical stimulation, upper-limb strengthening and psychosocial support.
The long-term direction, however, is important. As brain-computer interfaces become more accurate, wearable sensors improve, and powered exoskeletons become lighter and safer, future systems may offer more personalised control. This could eventually support patients not only in therapy rooms, but in daily environments where standing, transferring, stepping and assisted walking may improve independence.
For the IMEA region, the technology also raises questions about access. Exoskeleton rehabilitation requires specialist centres, trained therapists, maintenance support, safety protocols and careful patient selection. Countries building advanced rehabilitation services will need to consider not only the device purchase, but also training, clinical governance, reimbursement, service models and long-term technical support.
Why This Matters for O&P and Rehabilitation Professionals
Brain-controlled exoskeleton development matters because it expands how the sector thinks about mobility support after spinal cord injury.
Key implications include:
- Exoskeletons may support structured, repetitive gait training for selected SCI patients.
- Brain-computer interfaces could eventually allow more intuitive user control.
- Robotic rehabilitation may complement, not replace, conventional therapy and orthotic management.
- CPOs may increasingly work alongside engineers, neurologists, therapists and digital rehabilitation teams.
- Patient selection, safety, training intensity and clinical goals remain critical.
- Access and affordability will determine whether the technology reaches beyond specialist research centres.
For prosthetists, orthotists and rehabilitation teams, the message is clear: the future of mobility care will not be limited to passive devices. It will increasingly include powered systems, sensors, software, neurotechnology and patient-specific digital control.
- NR Times original article
- World Economic Forum / Reuters report on brain-controlled exoskeleton
- The Guardian report on the Grenoble brain-controlled exoskeleton trial
- Medscape report on brain-controlled exoskeleton in tetraplegia
- Systematic Reviews meta-analysis on exoskeleton robotics in SCI
- PMC full text: Exoskeleton robot training and SCI motor function
- World Health Organization rehabilitation overview