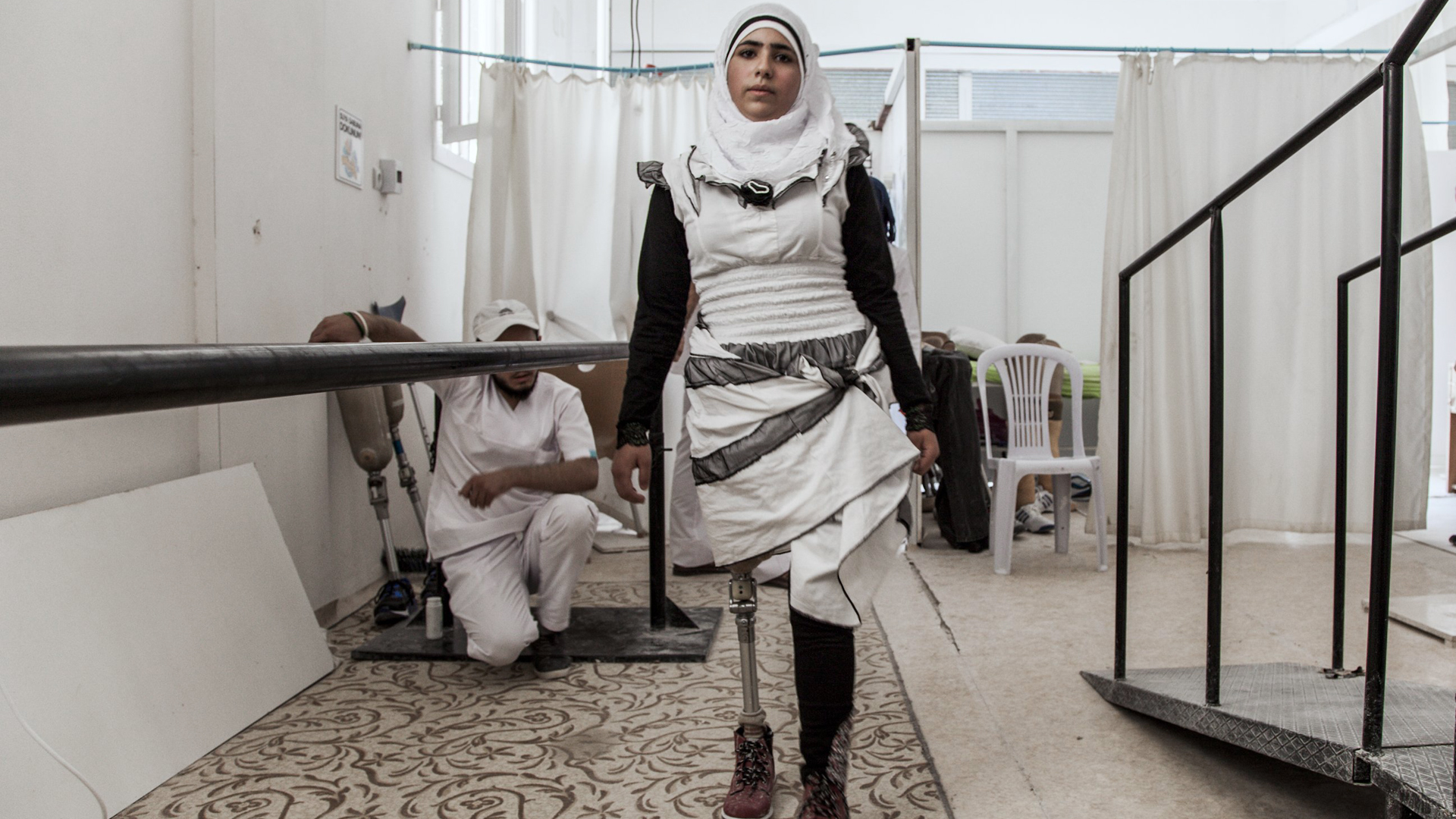
A recent article from The O&P EDGE has highlighted an important issue for prosthetics and orthotics: patients do not all experience limb loss, device fitting, rehabilitation or long-term prosthetic use in the same way. The article focuses particularly on differences between men and women who use prostheses, and points to a wider challenge for the profession — special populations require more specialised, individualised and clinically aware care.
The article cites data showing that women may wait longer to receive a prosthesis, have lower successful fitting rates than men, use their prostheses for fewer hours per day, and report higher levels of anxiety, depression, body-image concerns and residual-limb pain. These differences should be a warning to every O&P provider: standardised workflows built around the “average” patient may fail people whose needs, bodies, expectations and daily realities differ from the assumptions built into the system.
For the IMEA region, this discussion is especially relevant. Across the Middle East, India and Africa, O&P services often operate under pressure from limited staffing, high patient volumes, constrained budgets and uneven access to specialist rehabilitation. In such settings, there is a risk that device delivery becomes the main goal, while individual experience, gender, culture, occupation, body image, family role and psychosocial needs receive less attention.
Why Gender-Aware Prosthetic Care Matters
The O&P EDGE article quotes Jason Maikos, PhD, director of the VISN 2 Gait and Motion Analysis Laboratory at the VA New York Harbor Health Care System, who noted that what works for the average-sized man may not work for the average-sized woman. That statement should resonate strongly across clinical practice. Prosthetic design, socket configuration, component selection, suspension, alignment, cosmesis and rehabilitation planning all need to reflect the individual user.
Gender-aware care does not mean making assumptions about what women want. It means asking better questions.
For women using prostheses, key clinical considerations may include:
- Residual-limb shape, soft-tissue distribution and socket comfort
- Prosthetic weight and energy cost
- Cosmetic appearance and clothing choices
- Body image and emotional adjustment
- Pregnancy, postpartum changes or hormonal influences on volume
- Household, caregiving and work demands
- Safety, privacy and mobility in public spaces
- Access to female clinicians or culturally appropriate care where needed
- Pain, skin tolerance and prosthesis wearing time
- Confidence using a prosthesis in social, work and family settings
These issues are not peripheral. They can directly determine whether a prosthesis is worn, trusted and used in daily life.
Successful Fitting Is Not the Same as Device Delivery
One of the most important lessons from the article is that access to a prosthesis does not automatically mean successful rehabilitation. A patient may receive a device but still struggle with pain, socket discomfort, poor suspension, instability, social embarrassment, fear of falling or lack of confidence.
For O&P professionals, the measure of success should not be “was a prosthesis delivered?” The stronger questions are:
- Can the person use the device safely?
- Is the socket comfortable over a realistic wearing period?
- Does the device support the user’s work, family and community roles?
- Does the patient feel confident using it outside the clinic?
- Is the prosthesis acceptable in appearance and weight?
- Is follow-up available when problems occur?
- Does the user have access to repairs, adjustments and replacement parts?
In many low- and middle-income settings, the first fitting may be treated as the endpoint because resources are limited. But for the patient, it is only the beginning.
Special Populations Need More Than Standard Protocols
Although the O&P EDGE article focuses on women prosthesis users, the wider principle applies to many populations that require additional clinical attention. These include children, older adults, people with diabetes, bilateral amputees, upper-limb prosthesis users, people with traumatic limb loss, people affected by conflict, people with spinal cord injury, people with neurological conditions and individuals living in rural or low-resource environments.
Each group presents specific needs.
Children require growth monitoring, frequent refitting, school participation support and family education. Older adults may need lighter components, fall-risk assessment and careful management of comorbidities. People with diabetes may require skin monitoring, foot protection and prevention-focused orthotic care. Upper-limb prosthesis users need detailed functional training, realistic goal-setting and attention to device rejection. Conflict-affected amputees may need trauma-informed rehabilitation and long-term psychosocial support.
The common thread is that special populations are not “exceptions” to normal practice. They are a large part of real-world O&P care.
The IMEA Relevance: Culture, Gender and Access
In the IMEA region, gender-aware and population-specific O&P care must also account for cultural and access factors. For example, women in some communities may face additional barriers when seeking prosthetic or orthotic care, including transport limitations, family responsibilities, social stigma, cost, lack of privacy or limited access to female healthcare professionals.
A woman may delay care not because she does not need a prosthesis, but because the service model does not fit her life. She may need childcare, a female clinician, privacy during fitting, transport support, culturally appropriate cosmetic options or appointment times that do not conflict with family obligations.
Similarly, rural patients may struggle to attend repeated appointments. Humanitarian patients may be displaced before follow-up. Children may outgrow devices before replacements are available. Diabetic patients may require ongoing preventive care that is not reimbursed or easily accessible.
These are not soft issues. They are service-design issues.
What O&P Clinics Can Do Differently
O&P clinics and rehabilitation centres can improve care for special populations by making individualisation part of routine practice rather than an optional extra.
Practical steps include:
- Ask patients about daily life, not only clinical presentation
- Include questions about work, caregiving, school, household tasks and social confidence
- Record wearing time, pain, comfort and satisfaction at follow-up
- Offer gender-sensitive and culturally appropriate fitting environments
- Review cosmetic priorities without dismissing them as secondary
- Consider weight, ease of donning and doffing, and heat tolerance
- Build follow-up systems for socket discomfort and early device abandonment
- Use patient-reported outcome measures where possible
- Train clinicians and technicians to recognise bias in component and design decisions
- Include family education while still preserving patient autonomy
For special populations, small changes in clinical communication can significantly improve trust and outcomes.
Why Body Image and Mental Health Cannot Be Ignored
The O&P EDGE article notes that women prosthesis users report higher rates of anxiety, depression, worse body image and higher residual-limb pain levels. These concerns should not be treated as separate from prosthetic care. They influence prosthesis acceptance, wearing time, social participation and long-term rehabilitation outcomes.
A socket may be technically well made but still fail if the user feels embarrassed, unsafe, unsupported or disconnected from the device. A patient may reject a prosthesis not because they are “non-compliant,” but because the device does not meet their physical, emotional or social needs.
O&P professionals are not expected to replace psychologists or counsellors. However, they are often among the most important long-term clinical relationships for amputees and orthotic users. They can identify distress, normalise discussion, refer appropriately and design devices that better support confidence and participation.
Training the Next Generation of O&P Professionals
The article’s central message — that special populations require special skills — should influence O&P education and continuing professional development.
Training should include:
- Gender-aware prosthetic and orthotic assessment
- Paediatric-specific O&P pathways
- Diabetic foot and partial-foot management
- Trauma-informed rehabilitation
- Upper-limb prosthetic training and abandonment prevention
- Geriatric mobility and falls risk
- Cultural competence and communication
- Outcome measurement and patient-reported feedback
- Service models for rural and low-resource communities
In the IMEA region, this is especially important because many clinicians and technicians work across broad patient groups with limited specialist referral options. A practitioner may see paediatric orthotics, diabetic footwear, lower-limb prosthetics, spinal bracing and trauma cases in the same week. Stronger training in special populations can raise the standard of care across the whole system.
A Shift from Device-Centred to Person-Centred O&P
The future of O&P care must move beyond device delivery. The profession increasingly needs to judge success by function, comfort, confidence, participation and long-term use.
That shift requires a more person-centred approach. It means recognising that two patients with the same amputation level may require very different solutions. It means understanding that gender, age, culture, employment, family role, mental health, income and geography all shape rehabilitation outcomes.
Special populations do not need sympathy. They need better clinical systems, better questions, better follow-up and better design decisions.
Outlook
The O&P EDGE article is a timely reminder that prosthetics and orthotics cannot be built around a single default patient. Women prosthesis users, children, older adults, diabetic patients, conflict-affected amputees and other special populations all require more careful, individualised clinical attention.
For the IMEA O&P community, the message is clear: improving access is essential, but access alone is not enough. Patients need devices that fit their bodies, their lives, their environments and their identities.
The next stage of O&P development should be more gender-aware, culturally aware, outcome-focused and patient-centred. Special populations require special skills — and those skills should become part of everyday practice.
- Original article: The O&P EDGE – Special Populations Require Special Skills
- The O&P EDGE – Addressing the Unique Needs of Women Who Wear Prostheses
- Gender disparities in acquisition of lower extremity prosthetics following major limb amputation
- Gender differences in amputation outcome
- Gender differences in prosthesis-related outcomes among veterans
- Differences in prosthetic prescription between men and women veterans after lower-extremity amputation
- Living With Amplitude – Why do women wait longer for prosthetic care?
- WHO Rehabilitation 2030 Initiative